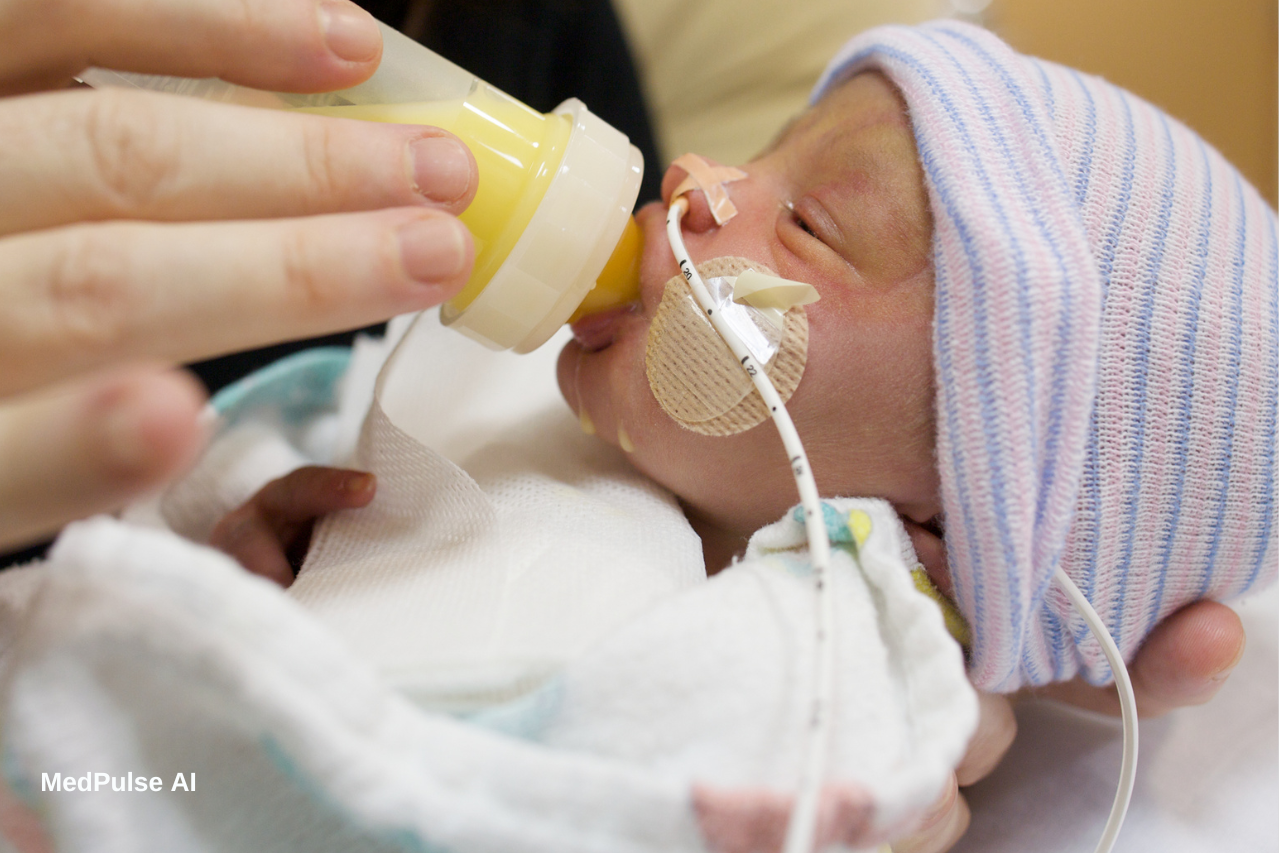
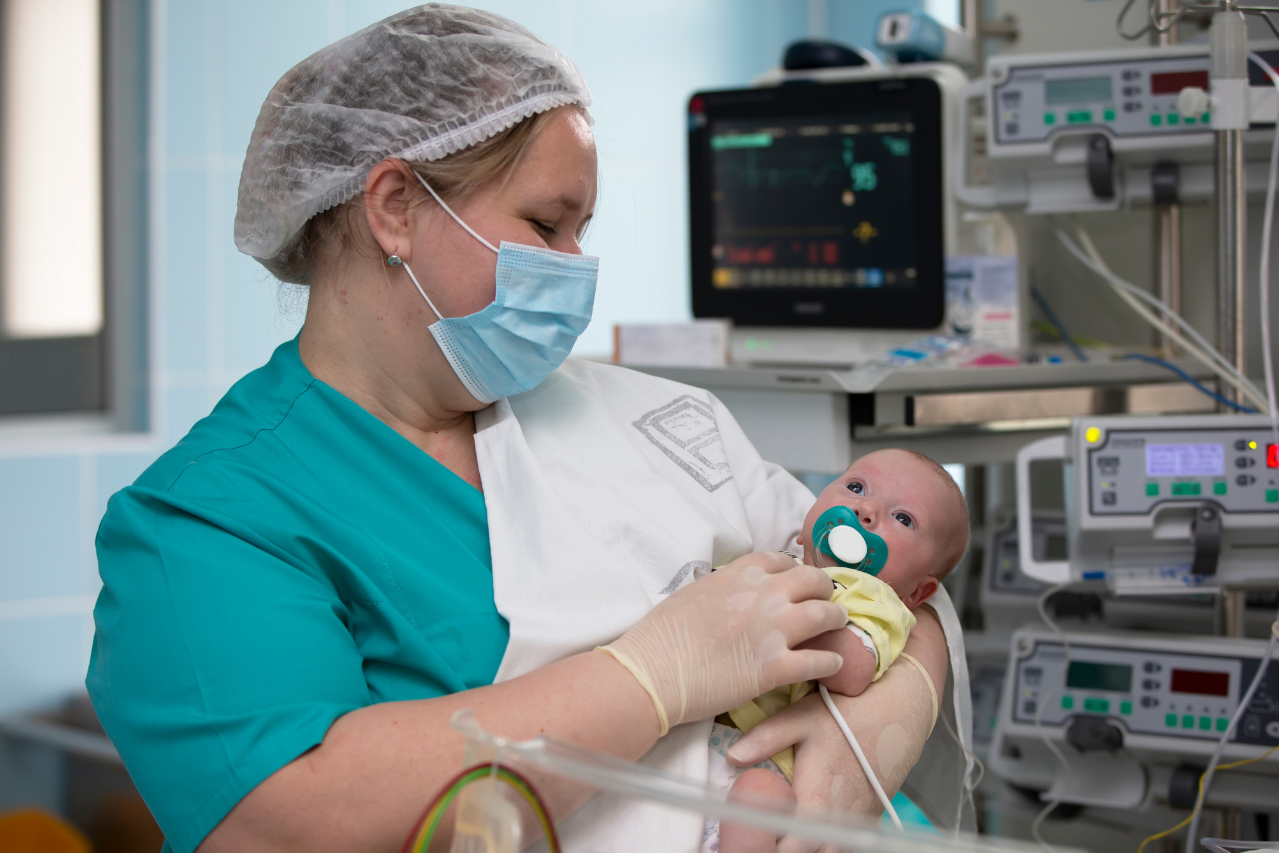
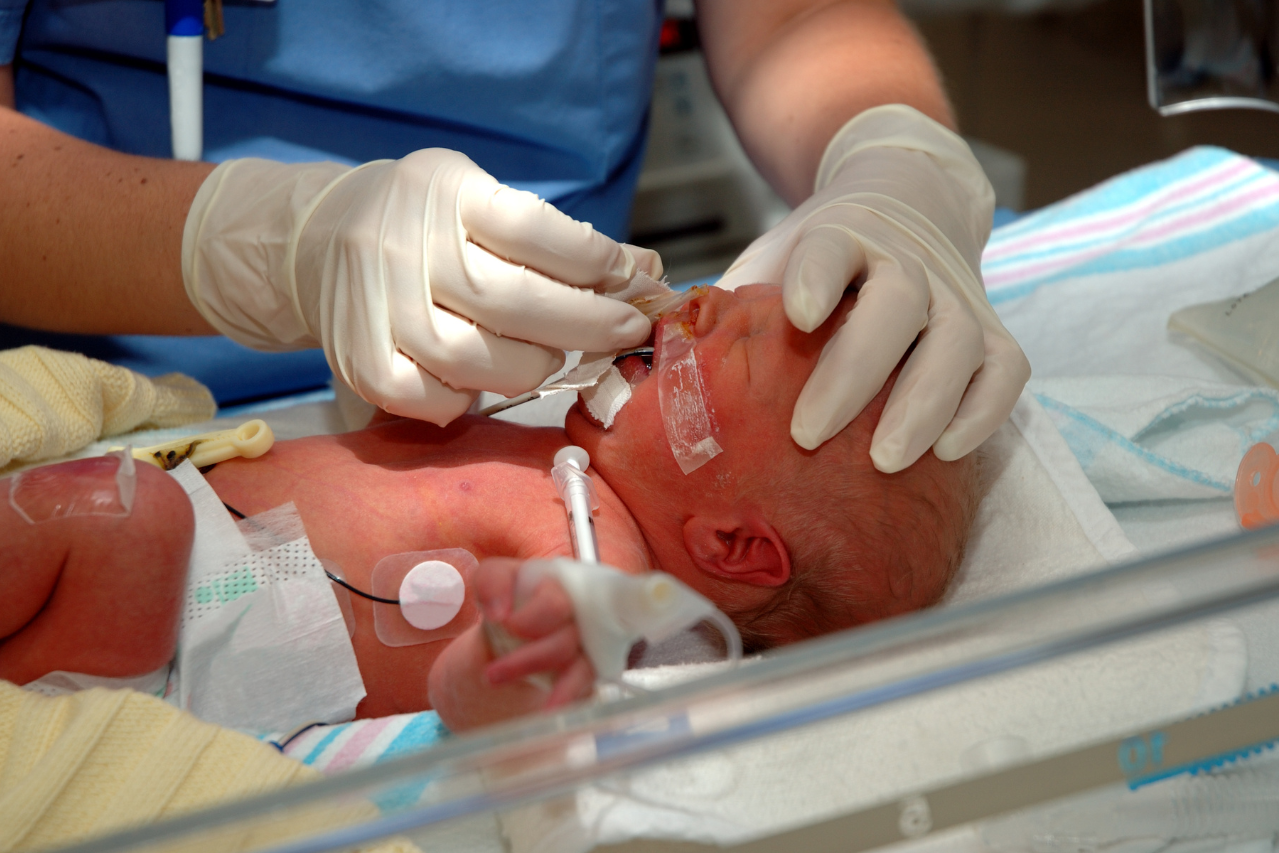
In neonatal intensive care units (NICUs), a baby’s life can depend on milliliters. For the tiniest patients—those born weeks too soon—nutrition isn’t as simple as a bottle or breast. It often arrives through an IV line, in a precisely formulated cocktail of proteins, fats, sugars, vitamins, and medicine. Getting that formula wrong can mean severe complications or worse.
A new study from Stanford Medicine, published March 25 in Nature Medicine, may change how we care for these fragile newborns. It shows that artificial intelligence (AI), trained on more than 10 years of NICU data, can design intravenous nutrition regimens that doctors often rate as better than those made by humans. And it might just transform global standards of care.
About 10% of babies are born prematurely. Those born eight or more weeks early often lack the gut development needed to absorb nutrients, making intravenous nutrition—known as total parenteral nutrition (TPN)—a critical intervention.
Yet TPN is notoriously complex. A typical prescription must be tailored daily based on a baby’s weight, lab results, clinical condition, and feeding tolerance. Six professionals may touch each order: a neonatologist, a pharmacist, a dietitian, and multiple nurses. Despite best efforts, the process remains manual, time-consuming, and error-prone.
“TPN is the single largest source of medical error in NICUs, both in the United States and globally,” said Dr. Nima Aghaeepour, the study’s senior author and associate professor of anesthesiology and pediatrics at Stanford.
And unlike feeding cues in healthy babies, preemies don’t cry when they’re hungry or stop when they’re full. Doctors have no real-time test to confirm if a baby received just the right amount of calories, micronutrients, or hydration.
Stanford’s AI model—called TPN2.0—was trained on 79,790 historical TPN prescriptions for 5,913 premature babies. It used data embedded in each child’s electronic medical record (EHR), including demographics, lab results, diagnoses, and outcomes. The algorithm learned to associate nutrition patterns with health outcomes—what worked, what didn’t, and for whom.
Here’s what’s striking: Rather than replacing daily prescriptions with a one-size-fits-all solution, the AI distilled all that complexity into 15 standardized formulas. Each baby could be matched to one formula, and the AI could adapt the choice daily as the baby grew stronger or developed complications.
In blinded tests, doctors preferred the AI-generated prescriptions over their own—and consistently. Even more important, babies whose real-life prescriptions diverged from what the AI would have recommended had higher risks of sepsis, bowel disease, and death.
“Sometimes imperfect data is good enough—as long as you have a lot of it,” Aghaeepour explained.
That’s the power of big data in clinical AI. Instead of relying on textbook-perfect nutrition or costly randomized trials, TPN2.0 learned from the messy realities of real NICU care—thousands of prescriptions, variable outcomes, different staff. It found the hidden patterns humans miss.
And the model held up when tested on external data: more than 63,000 nutrition orders from UCSF confirmed its generalizability.
Today’s TPN process is labor-intensive and resource-heavy. But if TPN2.0 becomes standard, hospitals could stock 15 ready-to-use IV formulas—preapproved, shelf-stable, and matched to each patient’s daily need via the AI engine.
This shift could:
- Reduce medical errors
- Free up clinicians to focus on patient care
- Lower costs
- Expand NICU nutrition access in low-resource hospitals
“This reflects our hope for how AI will enhance medicine,” said Dr. David Stevenson, a study coauthor and neonatologist at Stanford. “It will make doctors better and care more accessible.”
That accessibility matters. In many lower-income countries, custom TPN isn’t even available due to lack of expert staff or compounding pharmacies. A standardized AI-matched system could change that equation.
The Stanford team is preparing for a randomized clinical trial to test AI-prescribed TPN in live settings. But the AI won’t act alone—clinicians will still approve or adjust the recommendations, ensuring human judgment remains central.
“If something is missing from the record, the recommendation won’t be accurate,” said Dr. Shabnam Gaskari, chief pharmacy officer at Stanford Medicine Children’s Health. “We need a clinician to review it.”
But once approved, the AI-matched formula could be administered immediately—no waiting, no last-minute recalculations.
TPN2.0 represents more than a tool—it’s a glimpse into a future where AI isn’t an abstract add-on but an embedded partner in care. A system that doesn’t replace the nurse, pharmacist, or neonatologist—but makes their work safer, faster, and more reliable.
It’s a lesson in the power of good data, careful design, and clinical humility. And for thousands of premature babies each year, it might mean the difference between complication and recovery—between survival and a healthy start.